Who is eligible for blastocyst transfer?

Comprehensive Chromosome Scan
3 October 2022
When is pregnancy evident after embryo transfer?
3 October 2022Who is eligible for blastocyst transfer?
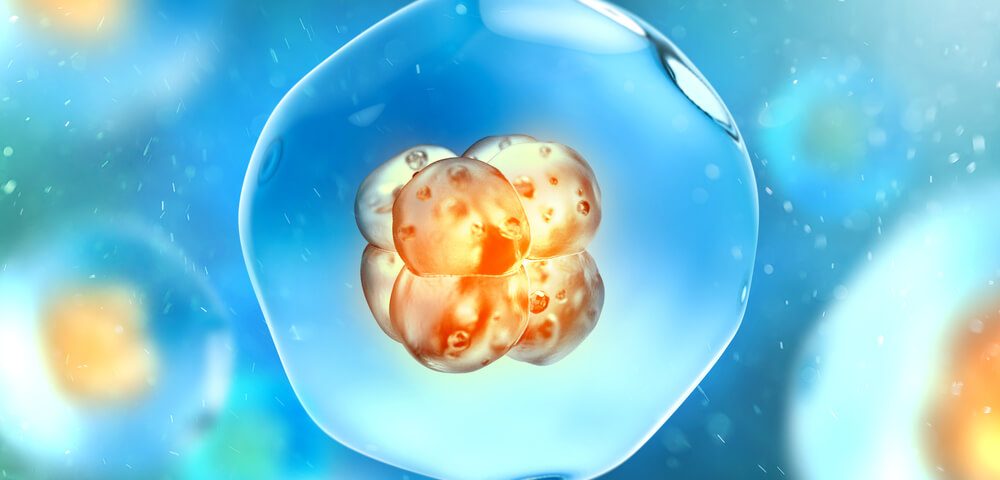
Who is eligible for blastocyst transfer?
To achieve a natural pregnancy, a woman and a man of reproductive age must have unprotected intercourse, the woman must be in the period of ovulation at this time, the egg and sperm must meet and fertilization occurs, and the resulting embryo must cling to the wall of the expectant mother’s uterus. If all these processes cannot be performed naturally, assisted reproductive treatments are used during pregnancy, and in vitro fertilization treatment is used as the most successful reproductive treatment. In IVF, a woman’s egg and a man’s sperm are combined in the laboratory, fertilization occurs, and the best and healthiest embryo is transferred to the uterus of the expectant mother.
A zygote, which is a single-celled embryo, is formed as a result of each fertilization, whether natural or through IVF. This first resulting embryo consists of a single cell, undergoes successive cell divisions and develops in the natural reproductive cycle. In a natural pregnancy, on the 5th-6th day of this process, the embryo moves through the tubes into the uterus. An embryo that develops continuously from the moment of formation is called a “blastocyst” during this period, that is, when it reaches the 5th or 6th day. The embryo at the blastocyst stage has a large volume, emerges from the surrounding membrane, called the “Zona pelucida”, and when suitable conditions occur, it attaches to the uterus and carries out pregnancy. This stage, which is called “implantation” and refers to the attachment of the embryo to the uterus, is carried out by transferring selected embryos into the uterus using special catheters that are removed by the doctor during in vitro fertilization procedures.
For more than 40 years, new and more effective methods have been discovered and used to make IVF treatment more successful. In the early years of in vitro fertilization treatment, embryo transfer was carried out in the early period of cleavage, that is, on the 2nd and 3rd days of embryo development, since there were not as many suitable media for the growth and development of the embryo as today. However, as the information and technical capabilities of IVF treatment and embryo development have increased, it has become possible to provide better development of embryos in the laboratory before implantation, that is, the attachment stage. For this reason, blastocyst transfer can be performed at different rates depending on the characteristics of the patient to be treated, the treatment history and the suitability of the clinical infrastructure, and pregnancy can be achieved with healthier and higher quality embryos.
Blastocyst transfer (embryo transfer on day 5)
Embryos that are created in the laboratory and developed by observation for 5 days, that is, which can live up to the 5th day in a viable and high-quality manner, are called “blastocysts”, the embryo transfer carried out on the 5th day is also called the “transfer blastocysts.” Scientific advances in IVF treatment have made rapid progress. In this context, one of the advanced technological applications is blastocyst transfer. This method gives couples who want to have children the chance to get pregnant much faster.
This treatment method is very important for couples who need IVF treatment, who are diagnosed with infertility, and who are afraid of multiple pregnancies. Many countries have introduced legal limits on the number of embryos transferred during IVF. In our country, in this context, this limit legally transfers a maximum of 2 embryos. Thus, when transferring embryos on the 5th day, that is, when transferring a blastocyst, 1 or 2 embryos that have reached the blastocyst stage are transferred to the uterus of the expectant mother, which reduces the risk of multiple pregnancy and increases the likelihood of pregnancy. However, since the likelihood of an embryo carrying any chromosomal abnormality reaching the blastocyst stage is much lower than that of normal embryos, day 5 embryos are known to be chromosomally healthier embryos. All this shows why blastocyst transfer is so important. Because the transfer of the blastocyst means higher implantation, that is, the likelihood of attachment and pregnancy.
The blastocyst stage is the healthiest stage of embryos!
Usually, in classical IVF, embryos are transferred to the uterus of pregnant women on the 2nd-3rd day, while with blastocyst transfer, the embryo can reach up to the 5th day, proving that it is healthy and of high quality. Embryos reaching the blastocyst stage are obtained on the 5th or 6th day after fertilization in the laboratory. After this period, Embryoscannot continue to survive in the laboratory and must be transferred into the uterus of the expectant mother without wasting time.
With IVF, 6-7 days after the transfer of the embryo, it leaves the zona pellucida, which is the protective layer of the embryo, and begins to attach to the uterine tissue. Embryos that have reached the blastocyst stage and are transferred later have a multicellular structure consisting of an inner cell mass that forms the fetus, a child, and trophectoderm cells that form the placenta. These embryos are limited by the quality of the inner cell mass and the structure of the trophectoderm. By transferring good quality embryos in both respects, a much higher pregnancy rate can be achieved. In addition, although more than one embryo has been obtained that can reach the blastocyst stage, they can be successfully frozen using vitrification, which is a method of freezing embryos, as well as successfully thawed and, if necessary, transferred to the mother’s uterus. Thus, it is possible to use high-quality embryos that reach the blastocyst stage after many years.
What functions should an IVF center have for blastocyst transfer?
- The technical equipment of the laboratory in which the processes will be carried out must be at a high level,
- The physical design, ventilation, cleaning and periodic control of all requirements of the laboratory must be carried out in full,
- Must have sufficient and high quality equipment for all kinds of problems that may arise,
- All necessary tools and equipment should be checked regularly,
- A professional and experienced team must be present in all aspects,
- Embryologists must be experienced in this field to seamlessly apply advanced techniques such as blastocyst transfer,
- Keep abreast of rapidly changing technological developments,
- Must be able to apply advanced in vitro fertilization techniques that will enhance the quality of the embryos.
To whom is the blastocyst transferred?
- The number of fertilized eggs in the laboratory is 7 or more,
- On the 2nd day, the quality of the embryo is better than normal,
- The age of the expectant mother is up to 35 years,
- The presence of 5 or more high-quality embryos on the 3rd day,
- Pregnancy did not occur despite receiving good quality embryos on day 2 or 3 in previous trials,
- Reluctance to have multiple pregnancies,
- Blastocyst transfer is done for couples who have received a large number of embryos but do not want their remaining embryos to be frozen.
What are the disadvantages of blastocyst transfer?
Blastocyst transfer is a technique that increases the overall success rate of IVF treatment.
However;
- It is undesirable for the expectant mother to be over 35 years old.
- The future father should not have serious problems with sperm.
- The more serious the cause of infertility experienced by a couple, the less likely it is that embryos derived from their cells will reach the blastocyst stage.
- In some couples, although Embryosare of good quality early in development, there may be serious problems with blastocyst development and may not develop. In such cases, treatment can be canceled without embryo transfer.
- The problem of developing embryos at the blastocyst stage can also vary depending on the technical infrastructure at the clinic where the procedure will be performed and the conditions such as air quality and hygiene required for the treatment.